Tendon and Bursitis Problems in the Knee
Common tendon problems in the knee include patella tendinopathy, Osgood-Schlatter disease and bursitis.
Patella tendinopathy
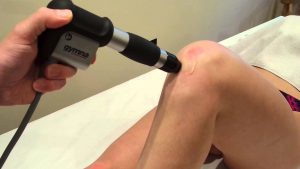
For patella tendinopathy we use gold-standard Shockwave Therapy which is one of the most advanced non-surgical and non-invasive treatment available for a wide range of stubborn conditions that are difficult to treat using a conventional treatment approach. Shockwave Therapy will preclude the need for steroid injections and invasive surgeries and enable rapid relief from your pain.
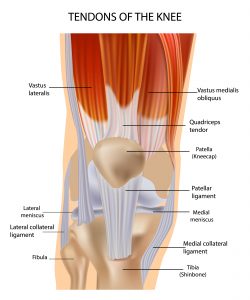
The quadriceps muscles coalesce to become a tendon that is known as the patella tendon. This tendon connects to your kneecap and then continues and inserts onto your shinbone. The patella tendon works in unison with the muscles in the front of your thigh (the quadriceps) to help straighten your leg.
Although anyone in principle can injure the patella tendon, tears are more common in middle-aged people who play any sport where running or jumping are strong components.
When tendons become stressed, they sustain small micro tears, this encourages inflammatory chemicals and the consequence is effusion (or swelling). This can quickly heal if managed appropriately.
However, if the load is continually applied to the tendon, damage occurring in the tendon can exceed the rate of repair. The damage may progressively worsen, causing pain and dysfunction. The result is a tendinopathy.
Research implicates that the cumulative microtrauma associated with high tensile and compressive forces generated during sport or related activities is a key determinant the evolution of tendinopathy. This occurs when cumulative microtrauma appears to exceed the tendon’s capacity to heal and remodel.
Shockwave Therapy is one of the most widely researched rehabilitation modalities, with increasing numbers of scientific studies added each year. The majority of research validates the effectiveness of extracorporeal shockwave. After only 3 or 4 treatments with shock wave, most patients report a significant reduction of pain and regaining of normal function.
Shockwave Therapy is so effective it is now recommended by the National Institute for Health and Clinical Excellence (NICE). NICE is an independent body set up in 1999 in order to provide the best evidence-based guidance and advice based on research and evidence about which treatments are most effective.
Osgood-Schlatter’s disease
Typical symptoms: This affects mainly teenage boys, causing a hard bony bump on the top of the shin. Pain will be evident just below your kneecap (patella) that is usually worse during, and just after, activity.
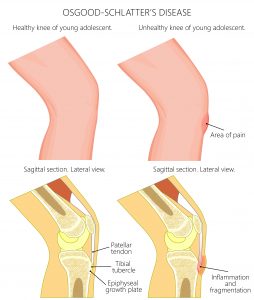
Osgood-Schlatter’s disease is a painful condition that affects the top of the shin bone (tibia). It typically occurs in active teenage boys who play sport. It causes pain and swelling below the knee. Sports that imply repeated and vigorous use of the muscles on the front of the thigh (the quadriceps) are thought to be a common causative factor.
The quadriceps muscle is used to straighten the knee. This muscle joins and pulls on the kneecap (patella), which pulls on the patellar ligament that attaches the kneecap to the shin bone (tibia).
Overuse of the quadriceps muscle creates repeated strain on the attachment of the patella ligament to the developing shinbone (or tibia). This can cause pain and soreness where the ligament attaches.
In some cases, a small flake of bone is pulled off the tibia by the pulling ligament (avulsion injury). The healing bone (callus) then forms which may cause a hard bony bump to develop although the actual knee joint itself is not affected.
The pain usually goes within a few months. It may help to be reassured that the condition is not serious and is likely to resolve.
Bursitis in the knee
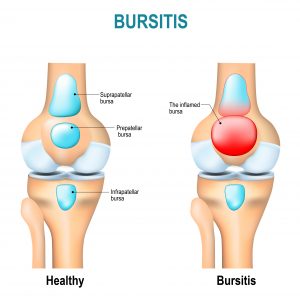
Bursae are structures that occur throughout the body and they are basically little sacks of fluid that typically occur between bony surfaces and overlying soft tissue (such as a tendon) and there are roughly 160 in the body in total. They essentially act as little cushions that help to prevent the effect of friction. However, ironically in the process of this duty they themselves can sometimes become irritated and inflamed.
Covering the kneecap is the prepatellar bursa. This can become inflamed by trauma to the front of the knee. This commonly occurs with prolonged kneeling. It is also known as ‘housemaid’s knee’, ‘roofer’s knee’ and ‘carpet layer’s knee.’
A second bursa lies underneath the kneecap and this is called the infrapatellar bursa and is often caused as a result of a jumping injury, hence the name ‘jumper’s knee.’
A third bursa of the knee is called the anserine bursa. It is located on the lower inner side of the knee. Anserine bursitis is particularly common in those who are over-weight. These patients can notice pain in the inner knee often while climbing or descending stairs.
Treatments for bursitis include:
- RICE treatment. You may find the swelling improves with (R)est, (I)ce packs, (C)ompression (wearing a bandage) and (E)levation.
- Anti-inflammatories
- Ultrasound and electrical treatment
- A steroid injection into the bursa may cure the problem
- Draining the fluid (aspiration) can be done with a needle and syringe if a lot of fluid builds up.